- Potentially Treatable Condition
- Muscles / Tendons / Ligaments / Cartilages
- Diabetic Foot Ulcer
- HOME
- ABOUT
- RESEARCH
- INSIGHTS & HAPPENINGS
- JOIN US
- CONTACT US
-

Diabetic Foot Ulcer: An open sore or wound that occurs in approximately 15% of patients with diabetes and is commonly located on the bottom of the foot.
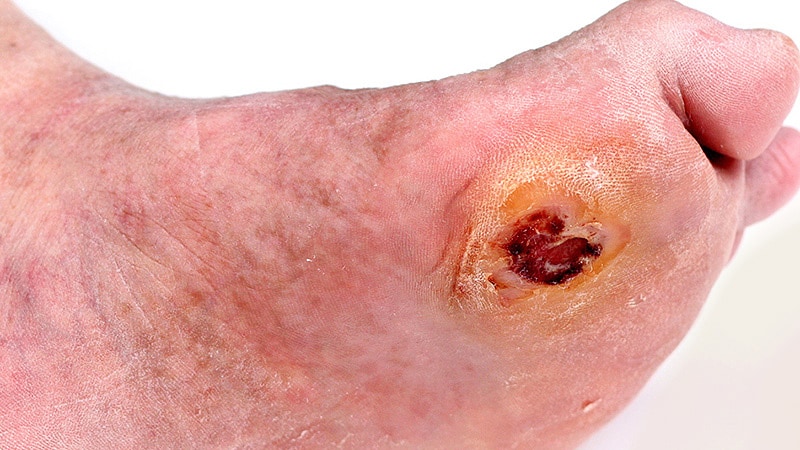
Diabetic foot ulcers usually begin with a foot injury, such as stepping on a nail or getting a blister from an ill-fitting shoe. This type of wound will typically heal on its own in people who do not have diabetes, but the situation is more complicated for those who do have diabetes.
Symptoms such as swelling, itching, and burning sensations can occur when a foot ulcer develops. However, if left untreated, it can deepen and worsen, resulting in serious complications. They are as follows:
When an ulcer develops on your foot or toe, you may notice changes in your skin such as:
As the ulcer worsens, it can become wider, longer, and deeper, even reaching the bone. In advanced stages, you might notice:
Ulcers form as a result of a combination of factors, such as lack of feeling in the foot, poor circulation, foot deformities, irritation, trauma and diabetes. Additionally, when high blood sugar levels damage the nerves and blood vessels in the feet, foot problems can develop over time. Damaged blood vessels can cause poor blood flow in your feet thus, the infection may not heal properly. There are two diabetic foot ulcers that are caused either by neuropathic ulcer or vascular ulcer.
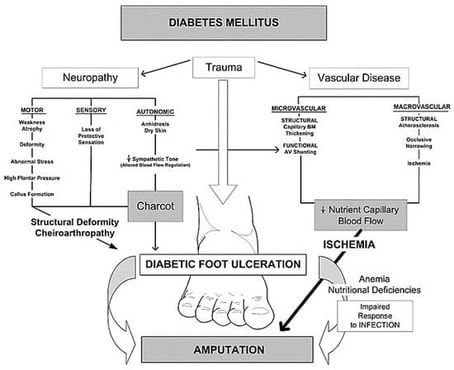
Neuropathic ulcer
Diabetic patients who have had the disease for a long time may develop neuropathy, characterized by a reduced or complete inability to feel pain in the feet due to nerve damage. High blood sugar levels can damage sensory nerves, resulting in peripheral neuropathy, which causes altered or total loss of sensation and the inability to feel pain. Peripheral neuropathy develops in approximately 50% of diabetic adults, increasing the risk of foot injury from pressure, cuts or bruises.
Vascular ulcer
Vascular disease can aggravate foot ulcer by impairing healing and increasing the risk of infection. Long-term high blood sugar levels can also damage blood vessels, reducing blood flow to the feet (ischaemia) or skin (microangiopathy) which can lead to delayed wound healing.
A doctor will first attempt to treat diabetic foot problems without using surgery. Some methods include:
When nonsurgical treatment does not successfully heal diabetic foot problems, a doctor might consider surgery. Surgical options include:

CelltiMax is Mesenchymal Stem Cells (MSCs) derived from human umbilical cords. Upon treatment, the cultured cells are injected intramuscularly / intravenously into the patient.
The cells are characterized by low immunogenicity. Hence, it is very safe, tolerable, and free of side effects. It has the capability to differentiate into specialized cells with specific functions for many parts of the body. They can reduce inflammation, repair, renew, regenerate, and replace damaged cells.
Improve bodies’ natural healing abilities
Modulate the immune system
Locate and reduce areas of inflammation
Replace damaged and diseased cells
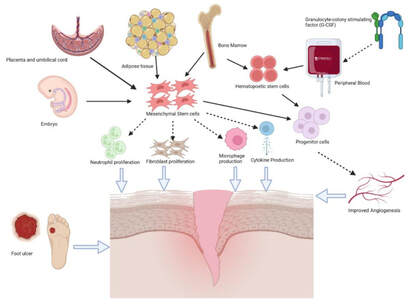
Among the therapeutic mechanisms of stem cells in diabetic foot ulcer healing include:
If you feel we might be able to offer meaningful improvement to both your condition and your quality of life, then please reach out to schedule a free consultation with one of our in-house clinical experts. We offer consultations in both Malay and English.





Review your medical history & recent evaluations
Explore what your treatment package might look like
Answer any questions you have about us
Answer any questions you have about the therapies
Discuss practical next steps, if you feel we can effectively treat you

Founded in 2010, Cell Tissue Group is a pioneering Malaysian medical technology company and a spin-off from the National University of Malaysia (UKM). As Malaysia’s first Tissue Engineering firm, Cell Tissue Group operates within a certified GMP Lab, ensuring the highest standards of medical research and product development, particularly in Tissue Engineering and Regenerative Medicine.



Founded in 2010, Cell Tissue Group is a pioneering Malaysian medical technology company and a spin-off from the National University of Malaysia (UKM). As Malaysia’s first Tissue Engineering firm, Cell Tissue Group operates within a certified cGMP laboratory, ensuring the highest standards of medical research and product development, particularly in Tissue Engineering and Regenerative Medicine.


Proudly powered by CTG © 2010-2026 Cell Tissue Group, a Universiti Kebangsaan Malaysia Spin-Off Company. – All Rights Reserved.